Stress Tests — Do You Need One?
Stress imaging tests cost approximately $1,000 each, and are used to measure blood flow to the heart and help determine how well the heart is working at rest and during exercise. The American College of Cardiology recommends that patients have the test administered two years after having a stent inserted, five years after bypass surgery, and sooner if a patient has chest pains or trouble breathing.
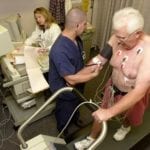 There has been a shift in recent years from hospital-based to office-based testing with more of the stress imaging tests being performed in doctors’ offices, instead of hospitals, as doctors purchase the equipment to do testing in their offices. Although cardiac stress testing performed in the office may result in quicker and more effect diagnosis, concerns have been raised about whether these tests will be overused in patients.
There has been a shift in recent years from hospital-based to office-based testing with more of the stress imaging tests being performed in doctors’ offices, instead of hospitals, as doctors purchase the equipment to do testing in their offices. Although cardiac stress testing performed in the office may result in quicker and more effect diagnosis, concerns have been raised about whether these tests will be overused in patients.
This issue is at the heart of the emerging litigation over Bracco Diagnostic’s CardioGen 82 imaging equipment, an office-based diagnostic machine for PET imaging that malfunctioned and led to the over-radiation of a number of heart patients around the country last year. Use of the PET imaging devices in cardiology offices around the country was suspended on July 26, 2011, by the FDA.
[youtube_sc url=”http://www.youtube.com/watch?v=sJTGyk6LxtY” playlist=” JAMA JAMAAuthorInterviews CORONARY ARTERY BYPASS CORONARY INTERVENTION PERCUTANEOUS ECHOCARDIOGRAPHY STRESS EXERCISE TEST NUCLEAR MEDICINE REIMBURSEMENT MECHANISMS” title=”JAMA%20Stress%20Tesing”]
There is a wide variation in whether a doctor prescribes a stress test where patients have no symptoms of coronary disease, at least according to a study by Dr. Shah published in the Journal of the American Medical Association (JAMA) in November of 2011. This researcher found that physicians who own equipment needed to administer a stress test ordered the test in 10% of their cases, while physicians who did not own the diagnostic equipment ordered these expensive tests in only 4.2% of their cases, suggesting the potential influence of a financial incentive in clinical decision-making. The rate of stress testing was highest among physicians who billed for both technical and professional fees (12.6%), followed by those who billed for professional fees only (8.8 %) and those who billed for neither (5 %).
This data suggests the need for broader application of the American College of Cardiology’s clinical guidelines to minimize the possible influence of financial incentives on the decision to perform cardiac stress testing on patients. Dr. Shah suggests that patients should ask their doctors about the purpose of each test and how it will help guide their treatment decisions.
As is always the case, informed patients receive better care at a lower cost and with greater efficiency by asking critical questions and taking charge of their healthcare decision making.
Share This


